Firm Mattress for Back Pain

If you are searching for a firm mattress for back pain, you are not alone. Back pain is one of the most common health complaints in the United States, and many people do not realize that their mattress may be contributing to the problem. Spending six to eight hours each night on an unsupportive surface can place continuous stress on the spine, discs, joints, and surrounding muscles.
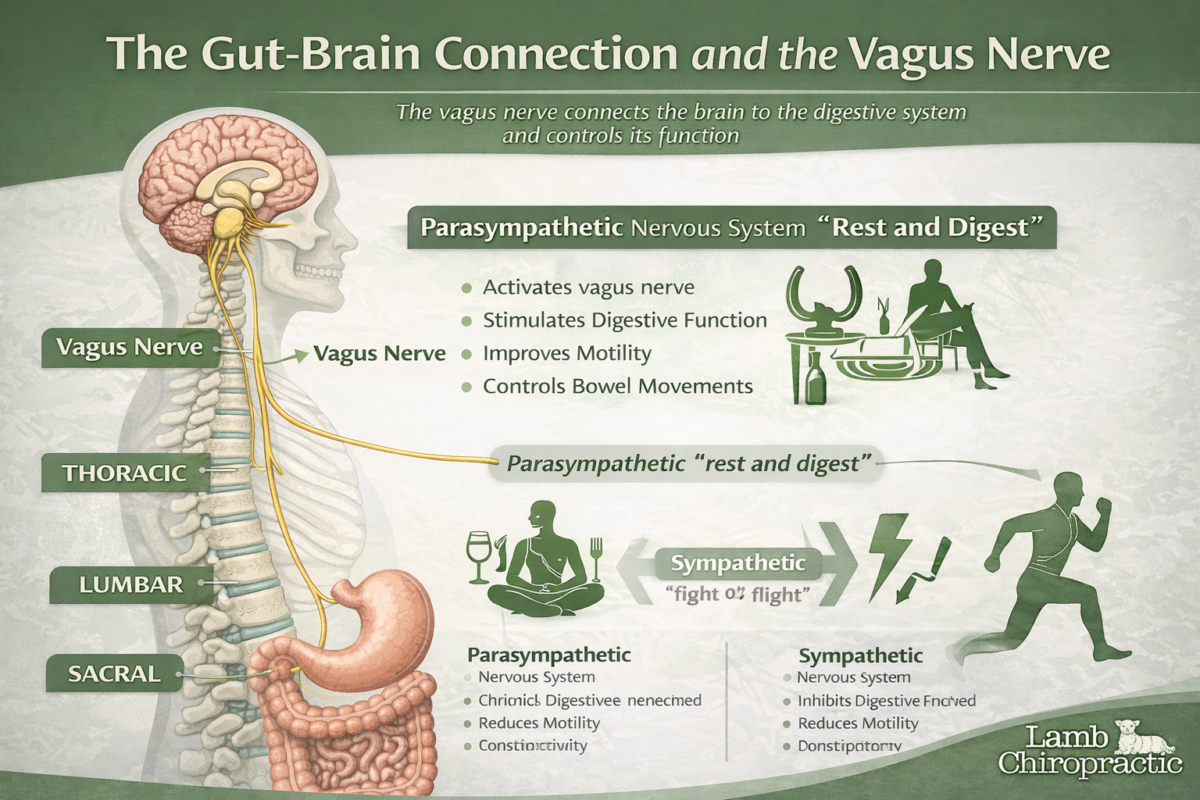
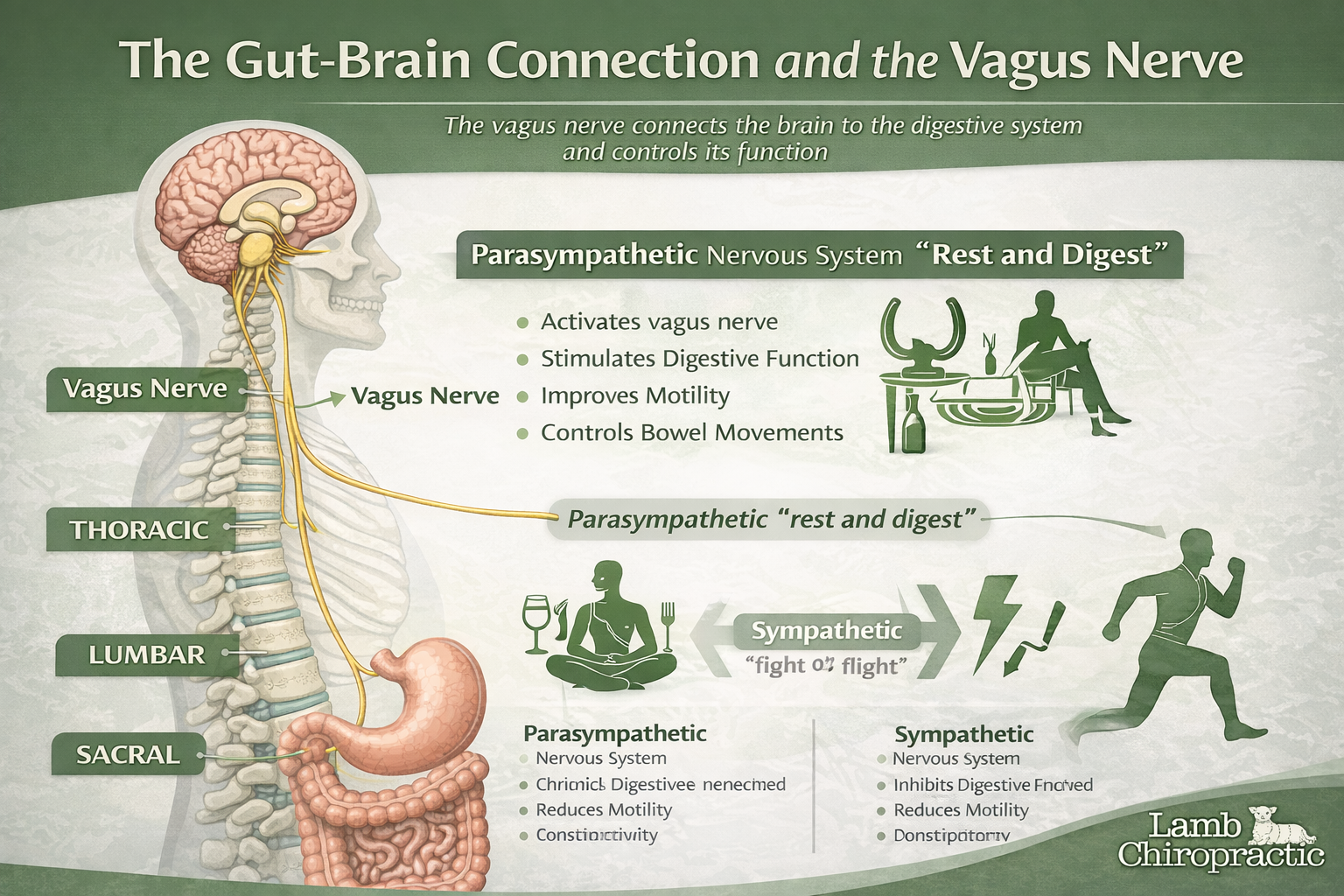
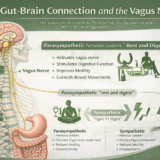
In my chiropractic clinic in Midtown Manhattan, patients frequently ask which mattress is best for back pain relief. While there is no single mattress that works for everyone, there are clear biomechanical principles that determine whether a mattress will help or worsen spinal problems. I always remind my patients of the five most important factors of health that need to be addressed. They are as follows (in no particular order): Diet, Exercise, Sleep, Proper connectivity between the brain and body via the nervous system, and a Positive Mental Attitude.
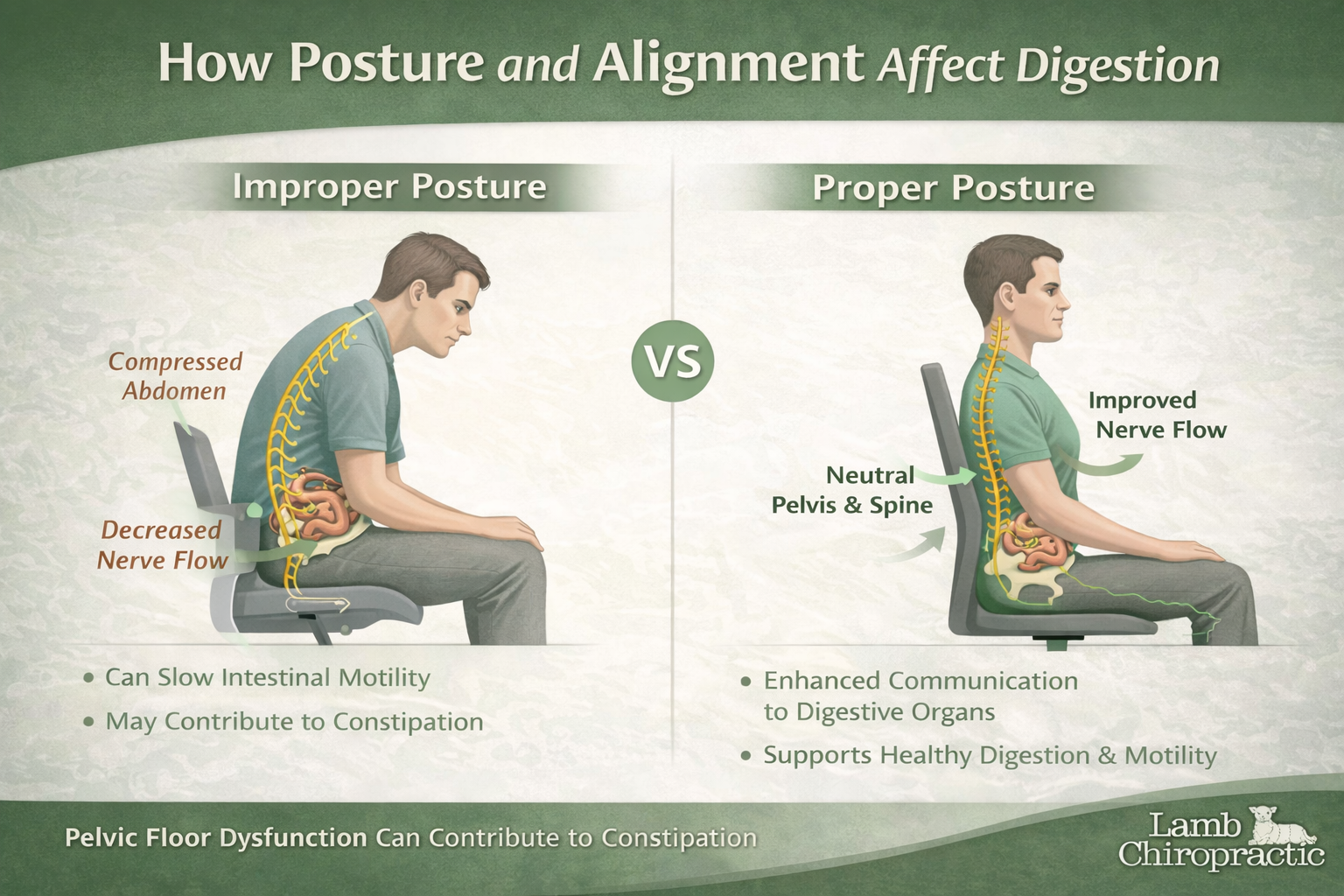
The goal of a mattress is simple. It should maintain the natural alignment of the spine while distributing pressure evenly across the body. When the mattress is too soft, the hips sink and the spine bends unnaturally. When the mattress is too hard without proper cushioning, pressure builds in the shoulders and hips.
For most people with back pain, the ideal balance is found in a firm or luxury-firm hybrid mattress that provides strong support from the base while still allowing slight contouring at pressure points. The right mattress can reduce pressure on your spine, improve sleep quality, and help your body recover overnight.
Why Mattress Firmness Matters for Back Pain
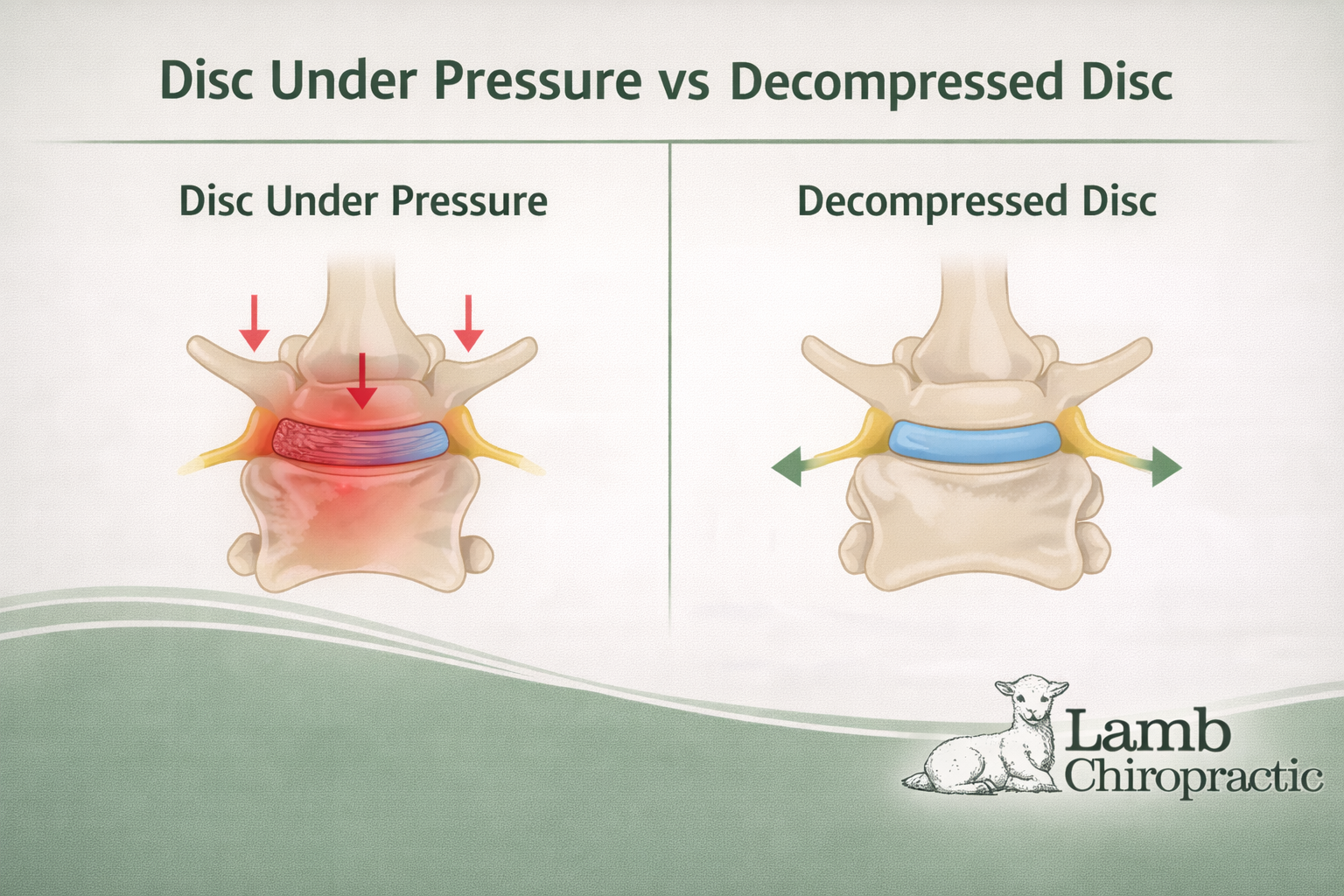
Your spine has natural curves in the neck, mid-back, and lower back. When these curves are supported properly during sleep, the muscles can relax and the discs can rehydrate overnight. When the mattress does not support these curves, several problems can occur. The hips may sink too deeply, causing the lower spine to bend forward. This increases stress on the lumbar discs and can aggravate conditions like sciatica or disc bulges. If the mattress is uneven or sagging, the spine may twist or bend sideways, which creates muscle imbalance and stiffness.
If the mattress is overly rigid without contouring support, pressure can build around the shoulders and hips. This often causes people to toss and turn throughout the night, disrupting sleep and preventing proper recovery. A firm mattress for back pain helps prevent these problems by stabilizing the pelvis and supporting the spine in a neutral position.
Mattress Types and Their Impact on the Spine
Not all mattresses are built the same. Understanding the differences between mattress types can help you make a better decision when choosing the best mattress for back pain. There are many good ones out there, but at Lamb Chiropractic, we consistently recommend Saatva mattresses for patients dealing with back pain due to their superior lumbar support and durability.
Memory Foam Mattresses
Memory foam mattresses conform closely to the body. This can reduce pressure points, but softer foam models sometimes allow excessive sinking, especially around the hips. High-density foam or firmer foam mattresses may work well for lighter sleepers, but they are not always ideal for heavier individuals who need stronger structural support.
Traditional Spring Mattresses
Traditional innerspring mattresses rely on coil systems for support. Older spring mattresses often create pressure points and uneven support because the coils move as a single unit. Modern designs have improved significantly, but traditional spring beds alone may lack the contouring necessary for optimal spinal alignment.
Hybrid Mattresses (Often Best for Back Pain)
Hybrid mattresses combine individually pocketed coils with foam or latex comfort layers.
This combination allows the mattress to provide:
Strong structural support from the coil base
Pressure relief from foam or latex layers
Better airflow and temperature control
Hybrid mattresses are often considered the best option for people looking for a firm mattress for back pain because they balance support with comfort.
Key Mattress Features That Help Back Pain
When evaluating mattresses, certain design features are particularly helpful for spinal health.
Zoned Support Systems
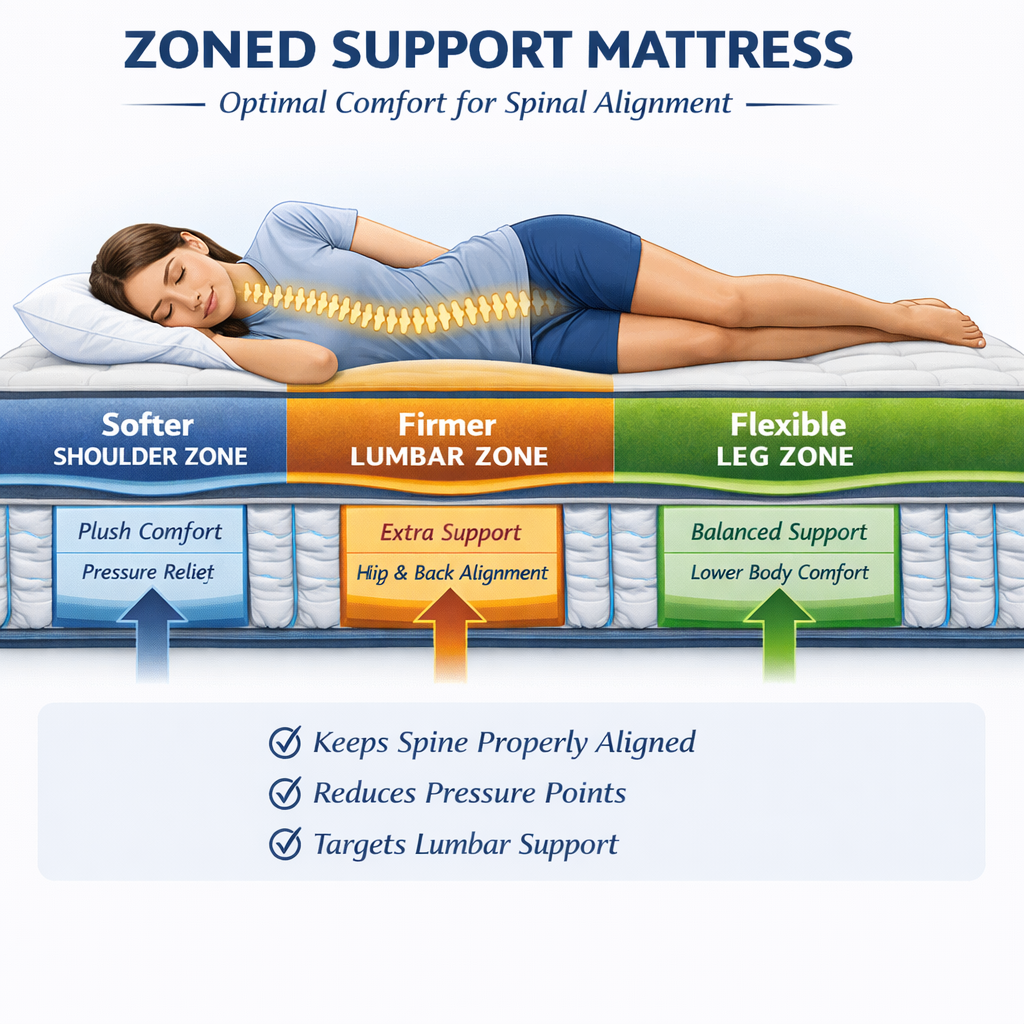
Zoned support means that certain sections of the mattress are firmer than others. The most important area is the center third of the mattress under the hips. Since the pelvis is the heaviest part of the body, firmer support in this region prevents the hips from sinking and keeps the spine aligned.
Hybrid Construction
Hybrid mattresses combine the stability of pocketed coils with pressure-relieving comfort layers such as latex or memory foam. This structure supports the spine while still allowing gentle cushioning for the shoulders and hips.
Firmness Level
For most adults with back pain, a luxury firm or firm mattress is the best choice. A mattress that is too soft allows the pelvis to drop and the spine to bend. A mattress that is too rigid may create pressure points. Luxury firm models typically provide the most balanced support.
Trial Periods and Delivery Policies
A mattress can feel very different after several nights of sleep compared to a few minutes in a showroom.
Look for companies that offer:
-Minimum 100-night in-home trial
-White Glove Set-up
-Free delivery and shipping.
-Free or low-cost returns
These policies allow you to test whether the mattress truly improves your sleep and back comfort. Mattress Firm has a 120 day return policy policy which is decent. Bloomingdales has a dynamic return and exchange policy that offers varying percentages back based on time. Saatva and Dreamcloud and a few others offer an exceptionally generous 365 day return poilcy.
Best Firm Mattresses for Back Pain

Many mattress companies now design models specifically with spinal support in mind. Below are several popular options worth considering.
Saatva HD and Saatva Rx
The Saatva HD and Saatva Rx are two of the best firm mattress options for people dealing with back pain.
These mattresses use durable coil systems combined with high-density comfort layers designed to maintain spinal alignment.
Saatva mattresses are made in the United States using the highest quality materials. They provide strong lumbar support and excellent durability.
Another advantage is that Saatva offers white-glove delivery, free setup, and 365 night in-home trial periods, which makes the purchasing process easier.
Because of their balance of support, durability, and quality materials, Saatva mattresses are often my top recommendation for patients looking for a firm mattress for back pain.
Plank Firm Luxe
The Plank Firm Luxe is designed for people who want an extremely firm sleeping surface.
It is a dual-sided mattress that allows sleepers to choose between firm and extra firm options. This can be beneficial for individuals who prefer minimal cushioning and maximum spinal support.
While not ideal for everyone, it can work well for stomach (please don’t sleep on your stomach) or back sleepers who need a very rigid surface.
WinkBed Firmer
The WinkBed Firmer is a durable hybrid mattress that offers significant firmness.
Its pocketed coil system provides strong lumbar support, making it a good choice for back sleepers or individuals who prefer a firmer feel.
The reinforced center support zone helps maintain alignment and reduces sagging around the hips.
Brooklyn Bedding Titan Plus
The Titan Plus mattress from Brooklyn Bedding is designed for heavier sleepers who require additional support.
It uses high-density materials and reinforced coils to prevent sagging over time.
For individuals with back pain who weigh more or need stronger structural support, this mattress can be an excellent option.
Avocado Organic Mattresses
Avocado mattresses are well known for using certified organic materials, including natural latex, organic cotton, and wool.
The Avocado Green Mattress and Avocado Latex Mattress both offer firm support and environmentally friendly construction.
For individuals who prefer natural materials, Avocado also offers latex toppers made from Talalay or Dunlop latex.
DreamCloud Premier Hybrid
The DreamCloud Premier Hybrid provides a balanced feel between firm support and cushioning comfort.
Its multi-layer hybrid construction makes it a good option for people who want support but still enjoy a softer top layer.
Helix Midnight Luxe
The Helix Midnight Luxe is another hybrid mattress designed to balance support and comfort.
While slightly softer than some firm models, its pocketed coil system and zoned support can still provide adequate spinal alignment for many sleepers.
Our patients can access exclusive discounts and white-glove delivery through this link to Saatva
Mattress Toppers for Back Pain
Sometimes a full mattress replacement is not necessary.
A firm mattress topper for back pain can improve spinal support and extend the life of an existing mattress.
Latex toppers are particularly useful because they provide resilience and support without excessive sinking.
Good options include:
Talalay latex toppers
Dunlop latex toppers
Eco-organic latex toppers such as those offered by Avocado
These toppers typically range between 2 and 3 inches thick, which is often enough to improve comfort while maintaining firmness.
Best Sleeping Positions for Back Pain

Your sleeping position plays a major role in how your spine is supported overnight.
Back Sleeping
Back sleeping is one of the best positions for spinal health. When combined with a supportive mattress and properly sized pillow, the spine remains in a neutral position. Placing a small pillow under the knees can reduce tension in the lower back. Unfortunately, many people have varying degrees of sleep apnea and cannot sleep on their backs for this reason. Others just do not find this position comfortable, but this would be the position of choice if it were possible..
Side Sleeping
Side sleeping is another healthy position when supported properly. Many experience shoulder pain while sleeping on their sides and subsequently seek alternative positions. A supportive mattress and pillow help keep the head, shoulders, and hips aligned. Side sleepers also can benefit from placing a pillow between the knees to maintain pelvic alignment.
Why Stomach Sleeping Is Problematic
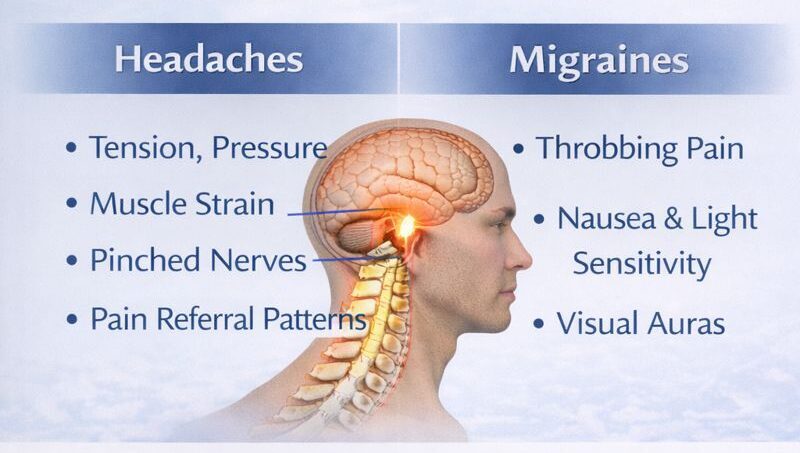
I never recommend stomach sleeping- unless you’re on a massage table with a cutout for your face. A “face-down” position forces the neck into prolonged rotation and extension, placing stress on the cervical spine and surrounding nerves. The twisting of the neck also causes torquing of the spine and spinal cord all the way down to the base. Over time, this can contribute to neck pain, headaches, and spinal imbalance. For patients with chronic neck or back pain, transitioning to back or side sleeping is usually much healthier.
The Importance of Proper Pillow and Positioning
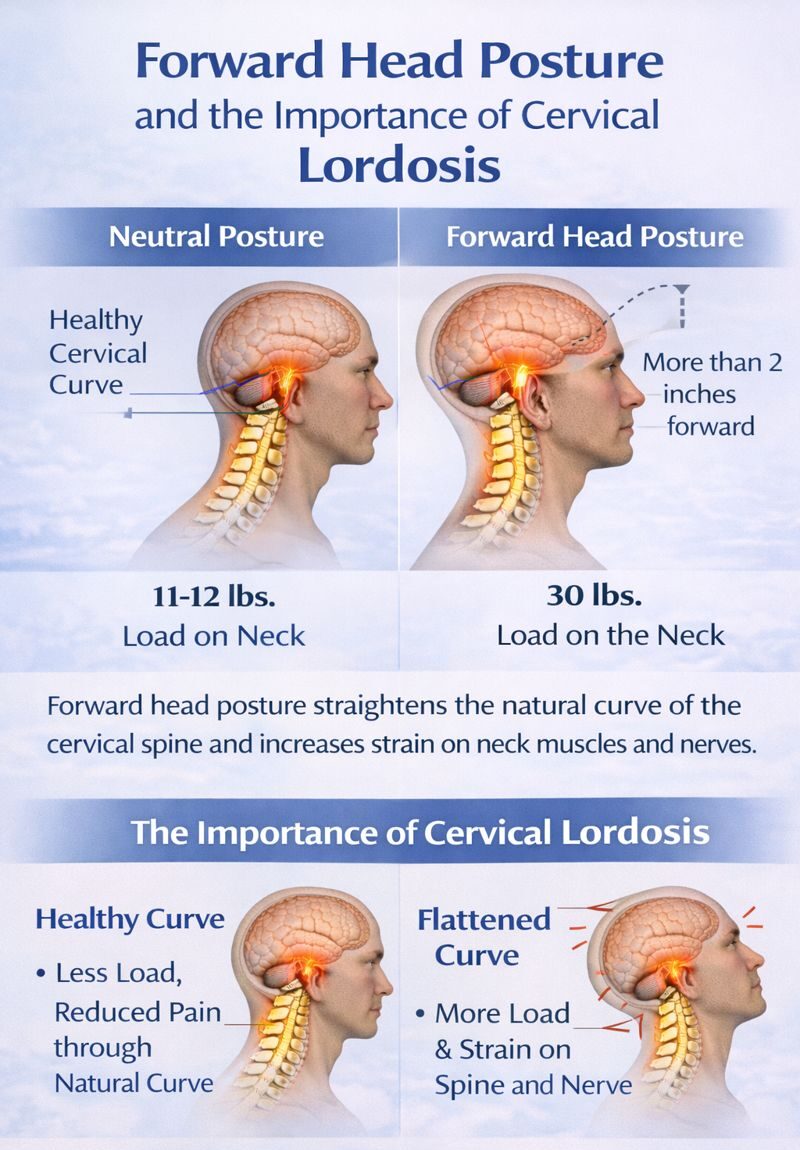
A mattress alone cannot correct poor sleeping posture. The pillow must also support the neck and maintain proper alignment between the head and shoulders. Too many pillows can force the neck forward, while too few can allow the head to tilt backward. Choosing the right pillow height is critical to maintaining a neutral cervical spine during sleep. It’s a good idea to use the camera on your phone in selfie mode to see how you actually are positioned on your pillow. If its too low (more common), try adding a folded up towel underneath until the proper height is achieved. Eventually, you will need a new pillow. If its too high, you will need a new pillow sooner than later. We will follow up with an article on pillows soon.
One of the most common things I deal with as a chiropractor is a loss of the normal cervical lordosis or curve in the neck. I give my patients corrective exercises in addition to performing postural corrections in conjunction with proprioceptive stimulation. Improving your posture in all areas of life is key. 6-8 hours of poor posture each night does not help.
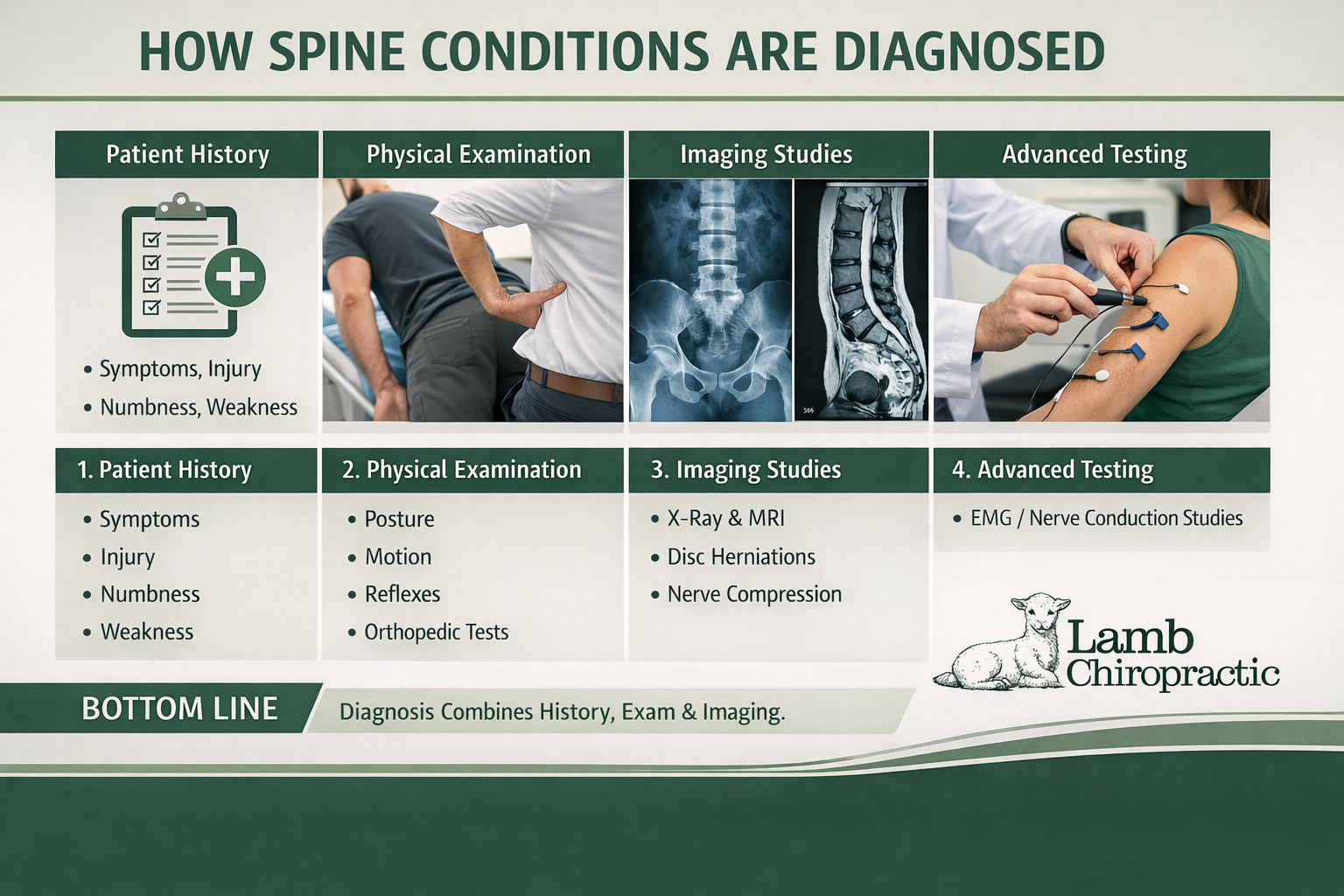
When Back Pain Requires Professional Care
While improving your mattress can make a major difference, persistent back pain may require professional evaluation.
Many cases of chronic back pain are related to:
Disc injuries
Spinal joint dysfunction
Muscle imbalance
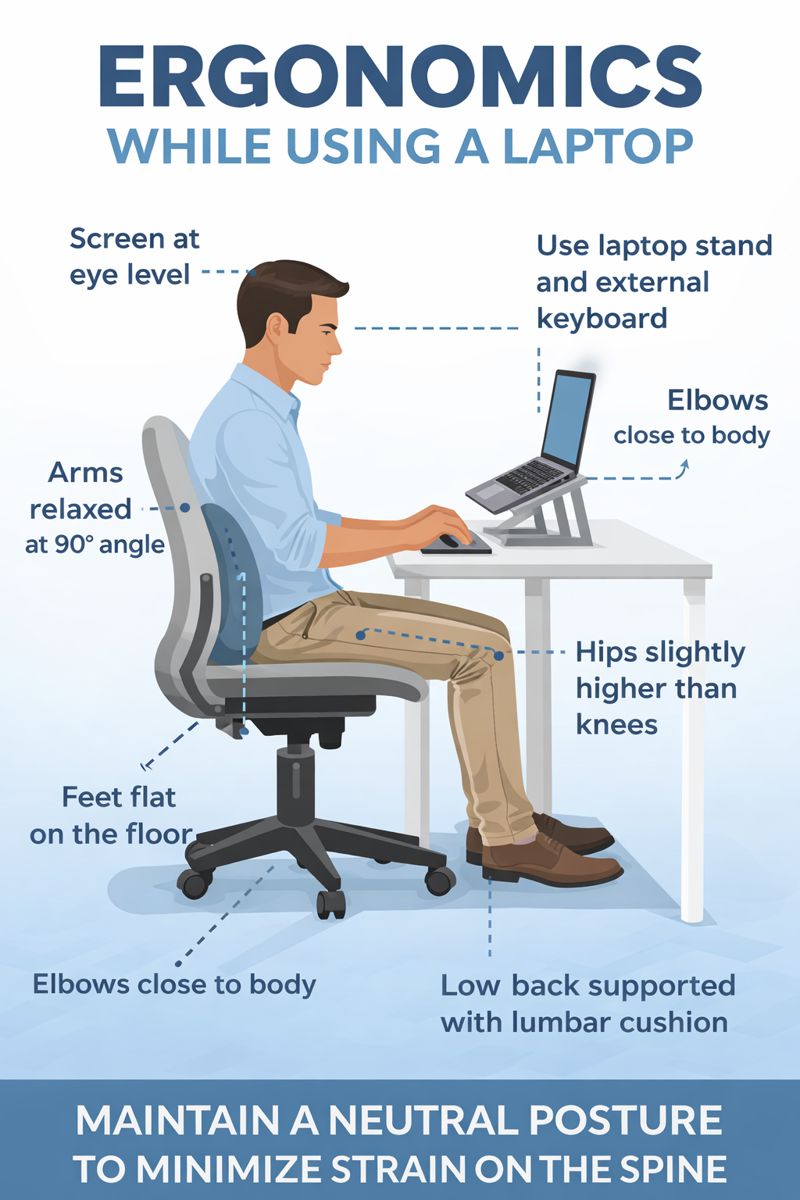
Poor posture or ergonomics
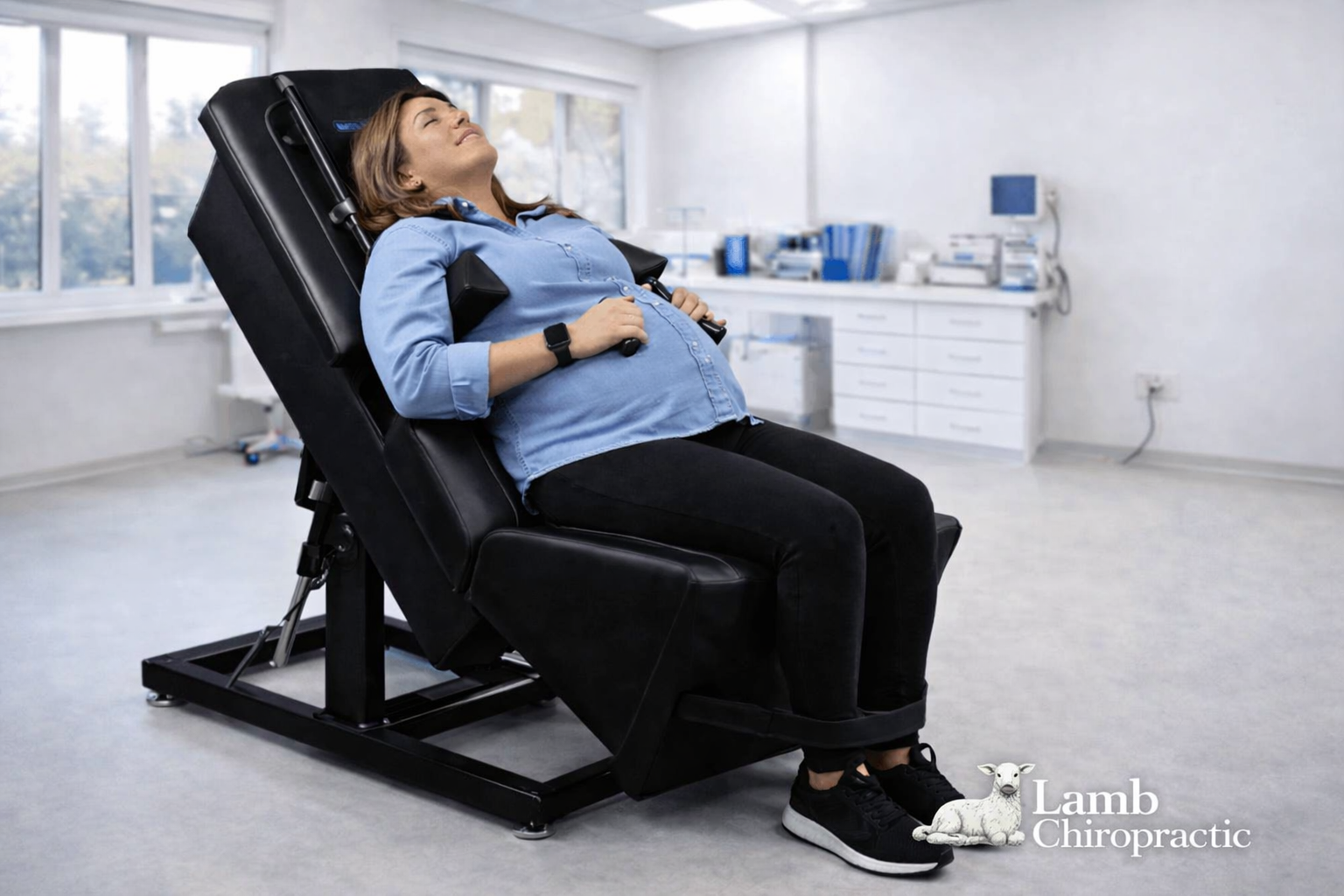
Chiropractic care, spinal decompression, mobility training, and lifestyle modifications can all play an important role in addressing the underlying causes of pain.
FAQ
Is a firm mattress better for back pain?
In many cases, yes. A firm or luxury-firm mattress helps keep the spine aligned and prevents the hips from sinking too deeply.
What firmness level is best for back pain?
Most people benefit from a luxury firm or firm mattress, particularly those with lower back pain.
Are hybrid mattresses good for back pain?
Yes. Hybrid mattresses combine coil support with foam or latex comfort layers, making them one of the best mattress types for spinal alignment.
Can a mattress topper help with back pain?
A firm mattress topper can improve comfort and support, especially if the underlying mattress is still structurally sound.
How long should a mattress last?
Most high-quality mattresses last 7–10 years, although durability varies depending on materials and body weight.
What is the best position to sleep in?
The answer is NOT on your stomach. Try to maintain a neutral position with your neck on your back or side.
Final Thoughts
Choosing the right mattress can significantly improve sleep quality and reduce spinal stress. A firm mattress for back pain with hybrid construction, zoned support, and durable materials can help maintain proper alignment throughout the night.
Combined with good sleeping posture, proper pillow support, and regular chiropractic care, the right mattress can play a meaningful role in improving spinal health and overall well-being.
Ready to Upgrade Your Sleep and Reduce Back Pain?
At Lamb Chiropractic, we frequently recommend Saatva mattresses because they combine luxury comfort with proper spinal support, especially for patients dealing with disc issues, sciatica, or chronic back pain.
The right mattress is not just about comfort. It directly affects your posture, recovery, and long-term spinal health.
Through our referral link, you can access:
-
Exclusive Saatva discounts
-
Free white-glove delivery
-
Risk-free in-home trial
👉 Click here to explore Saatva and claim your discount
Send us a message if you have any questions or would like to schedule your first chiropractic visit at Lamb Chiropractic in New York, NY!
Phone 212-883-8700
Email lambchiro@gmail.com
IG @lambchiro